PIB Backgrounder
India Speeding Towards TB Elimination
Posted On:
24 MAR 2026 6:59PM by PIB Delhi
Key Takeaways
- New cases of tuberculosis emerging yearly in India dipped by 21% from 2015-2024; mortality due to TB dropped by 28% during the same period.
- Under TB Mukt Bharat Abhiyaan, since 7th December 2024, over 20 crore vulnerable population is screened for TB, more than 28 lakh TB patients diagnosed.
- Over 46,118 Gram Panchayats have been awarded TB-free certification for the year 2024.
- New shorter, safer and highly effective BPaLM regimen having Bedaquiline, Pretomanid, Linezolid and Moxifloxacin has been introduced under the programme for drug-resistant TB patients.
- India's AI-driven TB programme uses AI to screen coughs, radiology AI to read chest X-rays, and predictive analytics to flag high-risk patients.
Introduction
World Tuberculosis Day
World TB Day is commemorated on March 24 to raise public awareness about the devastating health, social and economic consequences of TB. It reminds us to step up efforts to end the global TB epidemic. The date marks the day in 1882 when Dr. Robert Koch announced that he had discovered the bacterium that causes TB, which opened the way towards diagnosing and curing this disease.
|

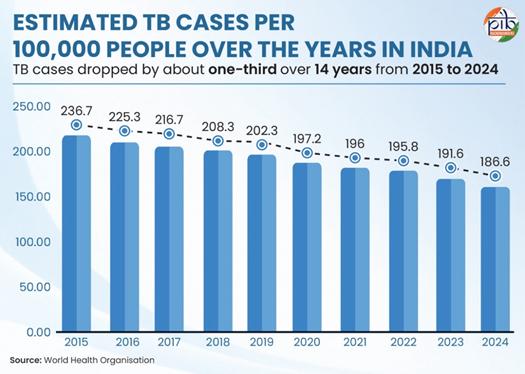
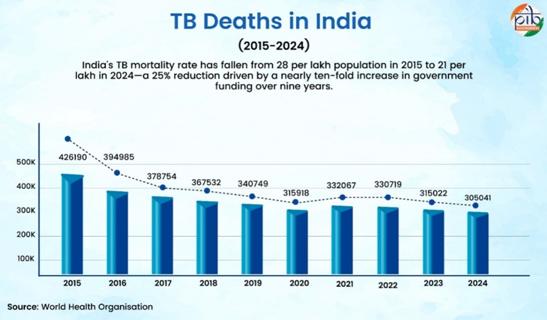
India is on track towards tuberculosis elimination. New cases of tuberculosis emerging yearly in India reduced by 21% from 2015-2024, according to the World Health Organisation’s Global Tuberculosis Report 2025. This marks one of the most significant declines in TB incidence globally, exceeding the pace of reduction recorded in other high-burden nations. Deaths due to TB reduced by 28% during the same period. The Government of India’s targeted, multi-pronged approach towards detecting, screening and treating tuberculosis has contributed significantly to this progressive trend.
Advanced technology expanded local health services, community engagement, and affordable treatment have put India on track to eliminate this prevalent and potentially fatal disease.
TB and Symptoms
What is Tuberculosis?
Tuberculosis (TB) is caused by a bacterium called Mycobacterium tuberculosis, usually impacting the lungs. TB can also affect other parts of the body, such as the brain, kidneys or the spine.
A person infected by the bacterium may become sick, but some do not. Inactive TB cases or latent TB infections also exist. People with inactive TB may not spread the disease to others like those with an active TB infection– yet they may develop active TB anytime and become sick. Babies and children, and people with weaker immune systems are more likely to get sick when infected. Without proper treatment, active TB can be fatal.
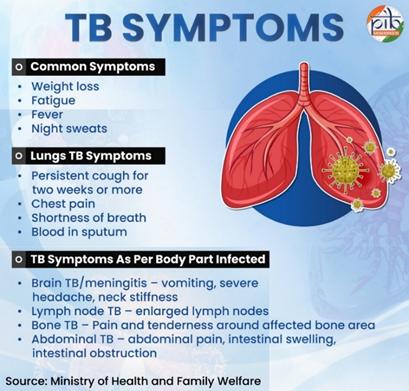
TB Symptoms
Symptoms of active TB are usually specific to the site affected by the bacteria, though there are some symptoms common to all types of TB.
People with active or symptomatic TB can spread the TB bacteria to others. When they cough, sneeze or speak, tiny droplets containing the bacteria can be released into the air and inhaled by people nearby—especially in spaces with poor ventilation.
Although tuberculosis spreads through the air, it does not transmit through:
- Handshakes
- Using public toilets
- Sharing food and utensils
- Everyday social interactions
Patients with lung TB generally stop being contagious after they have been on appropriate TB medicines for at least two weeks. People with TB in parts of the body other than the lungs usually cannot spread the disease.

Strategic Plan to End TB in India
The Government of India’s goal to end TB by 2025, in line with Sustainable Development Goal 3, is one of the world’s most ambitious health missions. The National Strategic Plan to End TB in India 2020-25, announced in June 2020, aims to eliminate tuberculosis through four pillars: Build, Prevent, Detect, and Treat. The plan focuses on early diagnosis, reducing transmission, treating patients with appropriate drugs and regimens, and creating patient support systems.

National Tuberculosis Elimination Programme
In 2020, the Government of India renamed the Revised National Tuberculosis Control Program (RNTCP) to the National TB Elimination Program (NTEP). This reflects India’s goal to eliminate tuberculosis before the global target of 2030.The NTEP builds on the four pillars of the NSP: Detect – Treat – Prevent – Build. The key activities of the programme are:
- Early diagnosis of individuals with TB through high quality testing, and proactive community outreach to find missing cases in vulnerable population.
- Prompt treatment with quality assured drugs and treatment regimens, including drug resistant TB.
- Engaging with patients seeking care in the private sector.
- Patient-centric treatment support and nutrition interventions through direct benefit transfer and Ni-kshay Mitra initiative.
- Contact tracing and TB preventive treatment among household contacts, children, PLHIV and in high risk /vulnerable populations.
- Airborne infection control measures.
- Multi-sectoral response for addressing social determinants.
The government runs various programmes under NTEP.
Pradhan Mantri TB Mukt Bharat Abhiyaan
The Pradhan Mantri-TB Mukt Bharat Abhiyaan (TB-Free India Campaign) was launched on September 9, 2022, as an additional key component of the NTEP.This initiative was launched to unite people from all walks of life in a ‘Jan Andolan’ (people’s movement) and accelerate the nation’s progress towards eliminating TB. Its objectives are:
- Provide Additional Support to TB Patients to improve treatment outcomes
- Augment Community Involvement
- Leverage Corporate Social Responsibility (CSR)
Nikshay Poshan Yojana and the Ni-kshay Mitra Programme
TB patients must eat a high-protein diet to counteract the adverse side-effects of the treatment drugs. The Nikshay Poshan Yojana, launched in 2018, provides financial assistance of Rs. 1,000 per month to each notified tuberculosis patient. Since its launch in April 2018, Rs.4,454.68 crores have been disbursed directly into the bank accounts of 1.38 crore beneficiaries.
TB treatment is long, lasting at least 6 months, and sometimes even longer. A Ni-kshay Mitra is a “TB Friend” or supporter who provides TB patients with help during this treatment period. A person, an NGO, corporations, religious and community groups, government officials and public figures can volunteer to be Ni-kshay Mitras.

Figure 1 - Ni-Kshay Mitras contribute food supplies to TB patients in Karnataka's Yelahanka's district (December 13, 2022), Ministry of Health and Family Welfare
The TB Friend provides regular food baskets to help patients reduce out-of-pocket expenditures. They can also provide psychosocial support by checking in regularly, and vocational support to help patients rebuild their lives after recovery.
As on November 12, 2025:
- 6,77,541 individuals and organisations have enrolled as Ni-kshay Mitras and distributed over 45 lakh food baskets to TB patients.
- Over 2 lakh My Bharat volunteers have come forward to serve as Ni-kshay Mitras. My Bharat is an initiative by the Ministry of Youth Affairs and Sports which connects 15-29-year-old people to various government departments, private organisations and civil-society partnerships to address real-world challenges and issues.
100-Day TB Mukt Bharat Abhiyaan
The Ministry of Health and Family Welfare launched one of India’s most intensive TB elimination drives called the 100-Day TB Mukt Bharat Abhiyan on 7th December 2024 in 347 high-priority districts across 33 States/UTs. To achieve early diagnosis of TB, vulnerability mapping and systematic screening of high-risk population for TB were undertaken. The Jan Andolan also led to active involvement of over 30,000 elected representatives and 24-line ministries and support of Ni-kshay Mitras exhibiting a whole-of-society and whole-of-government approach to TB elimination. The strategies of TB Mukt Bharat Abhiyaan have now been scaled up and expanded nationwide across all districts.
Under TB Mukt Bharat Abhiyaan, since 7th December 2024, over 20 crore vulnerable population is screened for TB, more than 28 lakh TB patients are diagnosed including 9 lakh asymptomatic cases, which could have missed otherwise.
As a result of all-round targeted and collaborative efforts, over 46,118 Gram Panchayats have been awarded TB-free certification for the year 2024.

The treatment success rate under the TB Mukt Bharat Abhiyan has risen to 90%, surpassing the global average of 88%.
New Initiatives
New shorter, safer and highly effective BPaLM regimen having Bedaquiline, Pretomanid, Linezolid and Moxifloxacin has been introduced under the programme for drug-resistant TB patients, which will reduce the duration of treatment to 6 months. More than 15,000 MDR/RR-TB patients have been initiated on this regimen.
TB Preventive treatment: Recognising that prevention is as critical as cure, TB Preventive Treatment (TPT) is provided to eligible beneficiaries to prevent the progression of TB infection to active disease. Through targeted and innovative approach, the programme has successfully protected household contacts and people living with HIV (PLHIV) over the years by administering TPT. The intervention has also been integrated with active and intensive case-finding campaigns and expansion to other vulnerable groups.

Ayushman Arogya Mandirs
Ayushman Arogya Mandirs are community health centres under the larger Ayushman Bharat scheme providing universal and affordable healthcare to all. There are 1,84,726 mandirs in India (as on March 24, 2026) – including sub-health centres, primary health centres, urban primary health centres, AYUSH (Ayurveda, Yoga & Naturopathy, Unani, Siddha and Homeopathy) centres and Urban Health and Wellness Centres. People showing TB symptoms can go to these centres to get diagnosed.

Figure 2 - Healthcare workers at an Ayushman Arogya Mandir in Himachal Pradesh's Kullu district screen women for TB and other diseases (September 20, 2025), Ministry of Health and Family Welfare
|
Technological Infrastructure
More than 9800 rapid molecular testing facilities and 107 culture and drug susceptibility testing laboratories exist – the world’s largest network – for early TB detection and care. Other tools are:
- Over 500 AI-enabled hand-held chest X-ray units for community screening, with 1,500 being delivered to the states and union territories
- Ni-kshay digital platform facilitates direct benefit transfer of nutritional support
Finding TB Cases in Remote Kashmir
In the isolated Gurez valley of Bandipora District, Kashmir—located 2,400 metres high in the Himalayas and cut off during winter—the NTEP Kashmir team conducted an intensive TB screening campaign. Using mobile testing vans equipped with advanced diagnostic machines and portable X-ray equipment, the team screened 1,250 people over three days and identified over 250 potential TB cases for further testing. They also conducted awareness sessions with the Indian Army, local health workers, village representatives, and religious leaders. This effort reflects Jammu and Kashmir's commitment to achieving a “TB Free Kashmir” by 2025.
AI-Led Initiatives
The government is using AI systems for the detection, diagnosis, and treatment of tuberculosis in its push to integrate the technology into healthcare delivery to improve access and speed of care. These are:
|
Health Focus
|
AI Solution / Initiative
|
Process, Technology & "Treatment" Experience
|
Clinical / Operational Impact
|
|
TB Screening
|
Cough Against TB (CATB)
|
Acoustic AI: A 3-second recording of a patient's cough via smartphone app analyses frequency patterns for TB signatures.[1]
|
1.62+ Lakh screened; 12–16% extra yield in cases over conventional methods.[2]
|
|
TB Management
|
Adverse Outcome Prediction
|
Predictive Analytics: AI flags patients at high risk of treatment failure, once flagged treatment is initiated.
|
Reported 27% decline in adverse outcomes after nationwide deployment.[3]
|
|
TB Triage
|
DeepCXR (Chest X-ray)
|
Radiology AI: Automated reading of digital X-rays to identify nodules/cavities for presumptive TB cases.
|
Deployed in 8 State/UTs; available free of cost to the Govt to bypass specialist shortages.[4]
|
Conclusion
India’s steady decline in TB incidence is a powerful reminder that sustained commitment, community participation, and strong public health initiatives truly make a difference. With continued vigilance, expanded access to care, and collective responsibility, the country is moving closer to a future where TB-free India is not just a goal, but an achievable reality.
References
Press Information Bureau:
· TB incidence in India drops by 21% from 237 per lakh population in 2015 to 187 per lakh population in 2024 – almost double the rate of decline observed globally: https://www.pib.gov.in/PressReleasePage.aspx?PRID=2189415
· World Tuberculosis (TB) Day – 2025: https://www.pib.gov.in/PressReleasePage.aspx?PRID=2114549
· TB is completely curable if right drugs are taken for the right duration - Director, National Tuberculosis Institute: https://www.pib.gov.in/PressReleasePage.aspx?PRID=1808582
· Mera Yuva Bharat: https://www.pib.gov.in/PressReleasePage.aspx?PRID=2184456
· India’s 100-Day TB Elimination Campaign: https://www.pib.gov.in/PressReleasePage.aspx?PRID=2081662
Others:
See in PDF
PIB Research
(Release ID: 2244661)
Visitor Counter : 5242